Endothelial function is a key marker of vascular health. It reflects how well blood vessels respond to physiological stimuli and plays a central role in conditions such as hypertension, cardiovascular disease, sepsis, and microvascular dysfunction. Importantly, endothelial dysfunction often occurs early—before structural changes or clinical symptoms become apparent—making it highly valuable for research and risk assessment.
For many years, the standard method to assess endothelial function has been flow-mediated dilation (FMD). FMD uses ultrasound to measure how much a blood vessel (typically the brachial artery) dilates in response to increased blood flow following a period of occlusion. While well-established, FMD comes with practical limitations: it is highly operator-dependent, requires specialized training and equipment, and can be difficult to standardize across sites or over time.
This is where Flow-Mediated Slowing (FMS) offers a compelling alternative.
FMS is based on a simple physiological principle. When endothelial function is intact, increased shear stress leads to nitric oxide release, resulting in vasodilation. This change not only increases vessel diameter but also reduces arterial stiffness—measurable as a decrease in pulse wave velocity (PWV). FMS captures this response using a standard blood pressure-style measurement, without the need for imaging.
Using the VICORDER®, FMS is measured oscillometrically in a fully operator-independent way. The procedure takes only a few minutes, integrates easily into study protocols, and produces reproducible results across different settings.
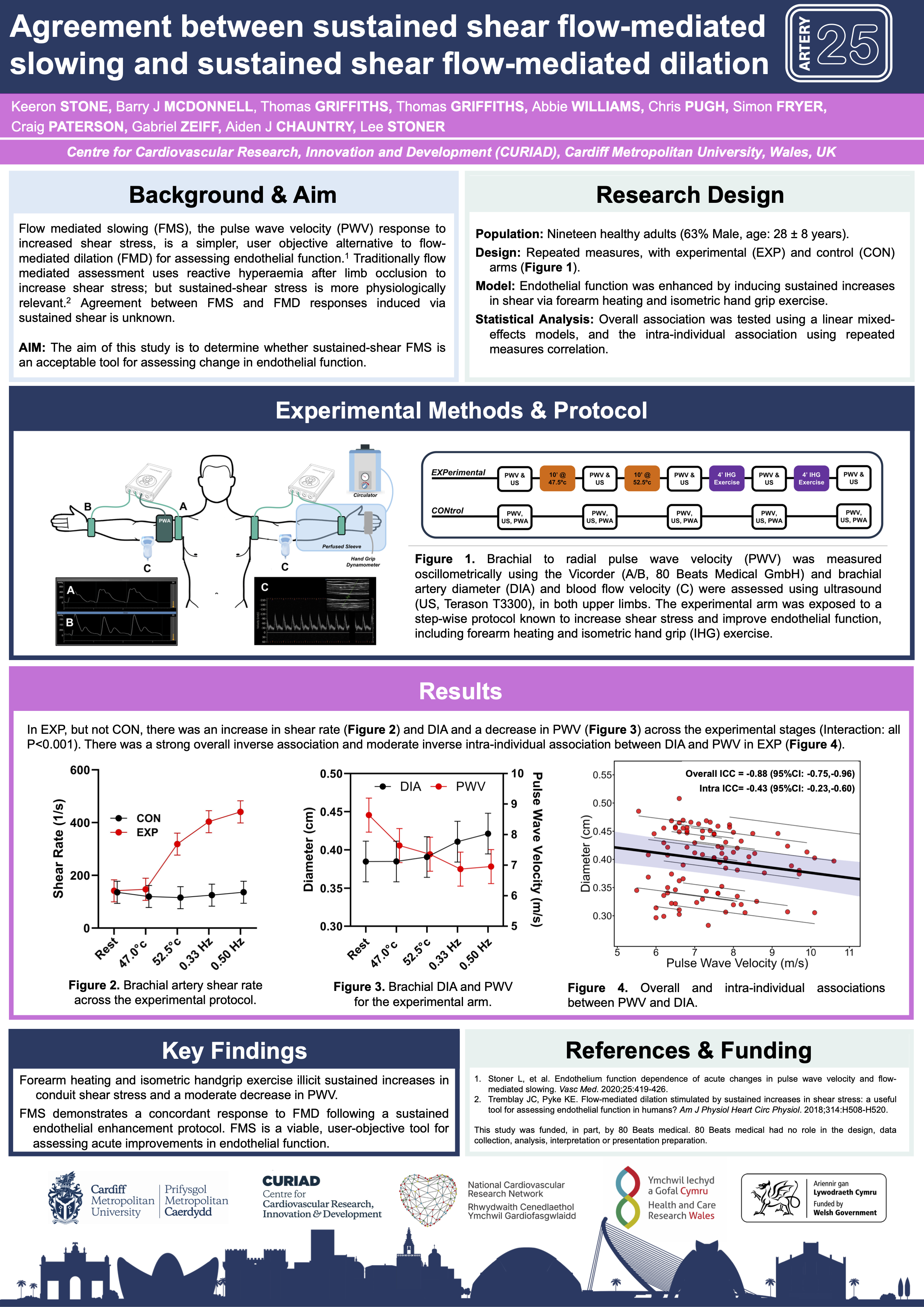
Recent data presented at ARTERY 2025 further strengthen the evidence base. The study demonstrates that FMS shows a concordant response to flow-mediated dilation under sustained shear stress conditions, with increased shear leading to arterial dilation and a corresponding decrease in PWV. These findings reconfirm earlier publications showing that FMS reflects endothelial function and is closely aligned with established FMD measurements
In practice, this means:
- No ultrasound or imaging expertise required
- Minimal operator dependency
- Fast, repeatable measurements suitable for longitudinal studies
- Easy integration into clinical workflows
FMS does not aim to replace FMD in all contexts, particularly where detailed imaging is required. However, it provides a powerful and practical alternative for studies and applications where simplicity, reproducibility, and scalability are essential.
With FMS, endothelial function assessment moves from a specialized procedure to a routine measurement—unlocking new opportunities for research and clinical insight.